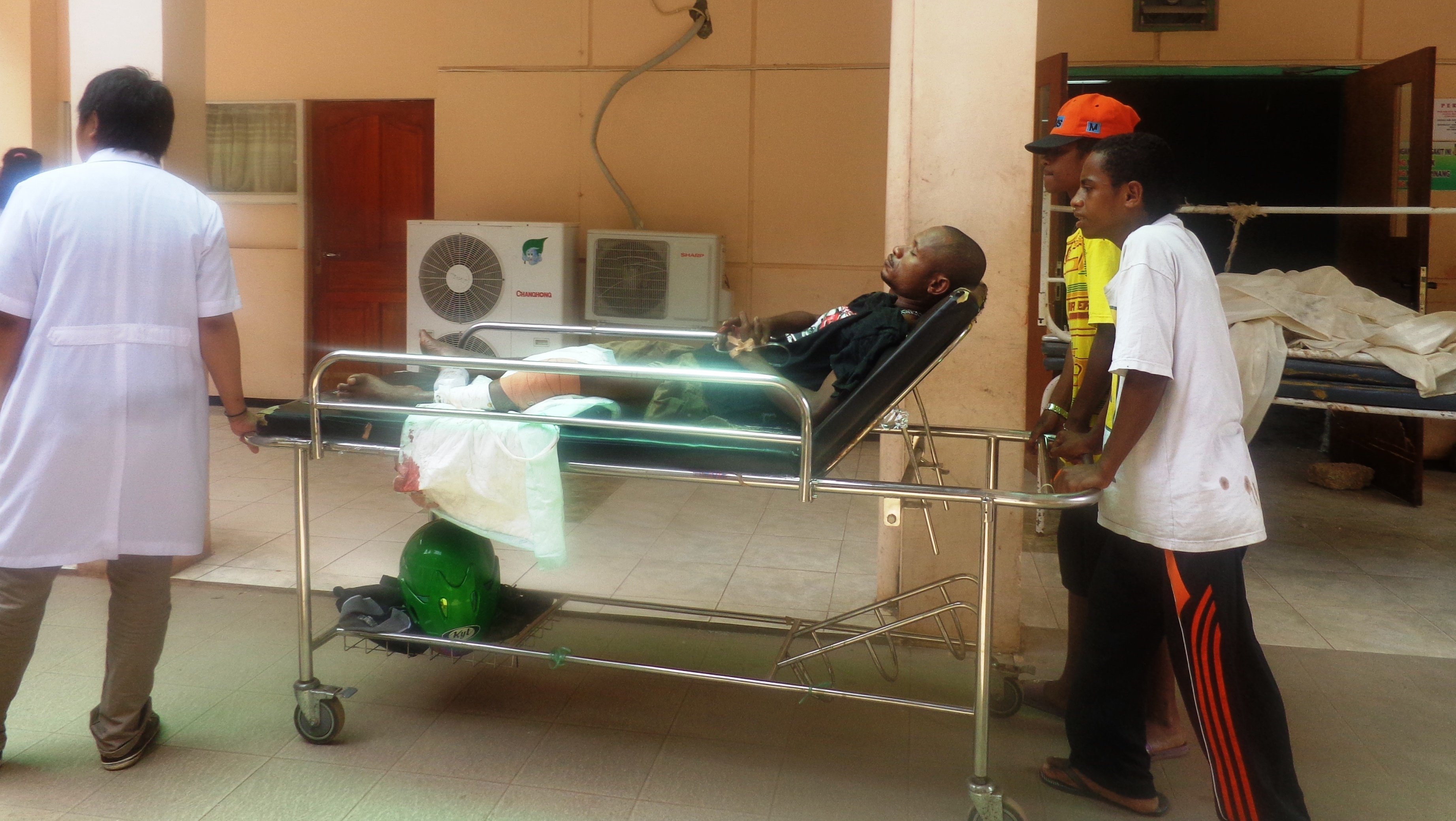
“People in the mountains and in coastal areas have flocked to the hospitals seeking treatment, even for diseases that can be handled by local clinics… People go straight to hospitals because they want to be treated by specialists,” said Aloysius Giay, director of the state-run Abepura Hospital near Jayapura, the provincial capital.
Yusmina Wakum pays around US$50 and travels 350km for eight hours by bus to reach the main hospital in Jayapura, to receive treatment for gout. “Where we live there's a hospital, but medicines are not good,” said Yusmina's 19-year-old sister, Miriam Wakum, as her elder sibling sat slumped in a wheelchair. “She got worse and couldn't sleep, so we decided to take her here.”
The health scheme was intended for use only in the province’s 34 tertiary referral hospitals, but residents have largely refused to seek care for non-emergency complaints in more than 300 public health clinics known as Puskesmas – citing poor service and lack of specialists – even though those services are also free, Giay said.
About 52 percent of Papua’s 2.8-million population are indigenous. In the past two years overcrowding has increased and patient queues have grown longer as more people joined the scheme, launched in 2009. The problem may worsen, health officials say, with the government’s plans to launch a universal healthcare scheme for all Papuans, indigenous and non-indigenous.
Health posts vacant
In Keerom district, near the border with Papua New Guinea, where violence from a low-level but long-running separatist conflict in Papua has fuelled security concerns, a local Catholic priest, Roni Guntur, said health posts are mostly vacant. “In some places the government has built community clinics, but there are hardly any health workers. Some of them left because they said there were no supporting facilities or because they did not feel safe.”
In 2012 Papua had a ratio of two doctors and 17 nurses per 10,000 people, above the national average of 1.4 doctors and five nurses, but Health Ministry data show that health personnel are not evenly distributed.
Some Papuan districts have less than one doctor and five nurses per 10,000 people, according to the Health Ministry, whereas the World Health Organization recommends a minimum of 23 health workers per 10,000 residents to provide basic care.
While reference hospitals in main towns like Jayapura and Abepura struggle to cope with the patient surge, many indigenous Papuans are still unaware of the health plan that is almost free of charge. “People in villages are still dying because they don't get treatment and aren't aware of their rights,” said Giay.
“Those who suffer more serious illness still have to pay for drugs because they are not covered by the insurance,” said the priest, Guntur, who noted that there was also confusion over what is covered by the insurance scheme.
Health consultations for indigenous communities are provided at no cost, as well as hospitalization in the cheapest, third-class ward and most medicines. Residents still bear transportation and some treatment costs.
Solutions
To cope with growing pressure on the health system, the provincial government has announced it will build four new referral hospitals in 2014. Officials said there are also plans to establish more schools for health workers, and to offer free training via the internet.
Most indigenous communities live in underserved remote areas, so in 2012 the Health Ministry started flying provincial health workers to these areas, where they stay for several months at time to treat villagers and train local health workers.
“Because of the limited budget, the provincial government can only provide [training] modules for the health staff, not for the local cadres, but by their own initiative the [provincial] staff developed very modest modules in the local language,” said Ratih Woelandaroe, a UN Children’s Fund (UNICEF) health officer in Papua.
The rugged jungle-clad landscape is the biggest challenge to accessing health services, said Sudhir Khanal, UNICEF’s child survival and development specialist in Papua.
Papuan Governor Lukas Enembe, installed in April 2013, has made improving healthcare a priority, and set up a Unit for the Acceleration of Health Care Development, which is headed by Giay.
"We are aware that all this time, monitoring and supervision has been poor, and that's why there's a need to make a move and improve things," Giay acknowledged.
apt/pt/he
This article was produced by IRIN News while it was part of the United Nations Office for the Coordination of Humanitarian Affairs. Please send queries on copyright or liability to the UN. For more information: https://shop.un.org/rights-permissions